Silicosis
Silicosis is the most common type of pneumoconiosis,
a progressive lung condition caused by inhalation of foreign substances
or dust and is characterized by nodular lesions. Left untreated,
pneumoconiosis can lead to fibrosis, where a condition marked
by the formation of excessive fibrous tissue, even after there
is no more exposure to the silica dust.
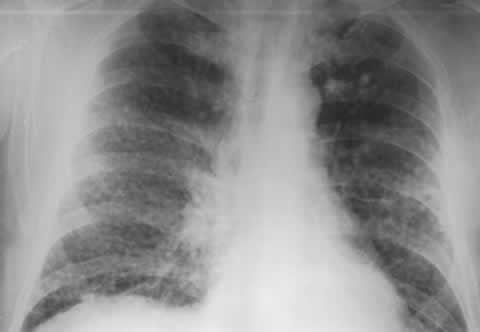
Silicosis showing as nodular mass on a chest x-ray.
Pathology
When silica particles are deposited in the lungs, a type of immune
system cell called alveolar macrophages will
ingest the compound in order to get rid of it. However, since
macrophages cannot process the silica compound, they will die
instead.
Dying macrophages release proteolytic or protein-degrading enzymes
into the surrounding tissue thus causing inflammation, which then
attracts other macrophages and a type of cell called fibroblast.
Fibroblasts are specialized type of cells that produce fibrous
tissues to isolate and wall off the inflammation, thus causing
nodules to develop in the lungs.
In silicosis, nodules typically develop in the upper lobes of
the lungs, near the terminal and respiratory bronchioles.
In most cases, silicosis only involves formation of the nodules,
which has no symptoms and is of no physiological significance.
However, in cases where there is a lot of fibrous tissue formation
or fibrosis, large areas of the lung can be destroyed.
Cause of Silicosis
Silicosis is the result of inhalation of silica dust, mainly
from industrial sources such as:
- Flint Ceramics
- Sandstone Building Material, Cement
- Silica Flour Materials in paint, porcelain, scouring soaps,
wood fillers
- Quartz Gold, lead, coal, and zinc mining

Electron microscopy of silica dust.
People who are most likely to develop silicosis are those who
are continually exposed to silica dust due to their working environment.
These include:
- Foundry workers
- Miners
- Stonecutters
- Grinders
- Boiler scalers
- Sand blasters
- Tunnel workers
Classification
Silicosis is classified according to its severity, onset and
rapidity of progression of the disease. It usually begins as an
asymptomatic (with no symptoms) condition, which can then develop
into:
- Acute silicosis
This form of the disease develops after 1 to 3 years of exposure
to very high concentration of silica dust.
- Accelerated silicosis
This form develops at an average of 10 years of lower concentration
of silica.
- Chronic silicosis
Simple and complicated silicoses develop after 20 years or longer
of exposure to lower levels of silica.
Symptoms of Silicosis
In early stages, there may be no symptoms of silicosis. The disease
can then progress to develop the following symptoms:
- Dyspnea (air hunger) or difficulty in breathing,
especially after physical exertion
- Tachypnea or rapid breathing
- Persistent dry cough
- Hoarseness
- High blood pressure or pulmonary hypertension
- Confusion
- Tiredness, lethargy, or malaise
- Difficulty in sleeping
- Changes in breathing characteristics (decrease in rate and
depth of breaths)
- Heart failure
- Cor pulmonale or enlargement of the right-side
of the heart
Diagnosis
In addition to confirming the patient’s current and past
occupation as a risk factor, diagnosis of silicosis include:
- Physical checkup
Chronic silicosis reveal decreased chest expansion, diminished
intensity of breath sounds, crackling, and rapid breathing.
- Chest x-ray
Small and discrete nodules are present in chest x-ray of simple
silicosis. In advanced cases, large masses of dense, fibrous
tissue are seen.
- Pulmonary function tests
These tests will reveal reduced lung capacity in silicosis patients.
Treatment
There is no cure for silicosis, instead treatments of this condition
focus on supportive or palliative measures. These include:
- Limiting exposure to lung irritants and smoking cessation
- Cough suppressant
- Inhaled bronchodilators to make breathings easier
- Chest physiotherapy
To help with coughing and bronchial drainage of mucus, physiotherapy
techniques such as chest percussion or vibration (gentle tapping
of the chest) can be done.
- Increased drinking water consumption (at least 3 quarts or
liters per day)
- Oxygen administration
To avoid hypoxemia or insufficient oxygenation
of the blood, oxygen can be administered by cannula or mask.
Patients with severe silicosis may require mechanical ventilation.
- Antibiotics in cases of respiratory infections
Complications
Silicosis can develop into more serious conditions, such as
pulmonary tuberculosis (TB) and fibrosis, which
can cause respiratory insufficiency and cor pulmonale.
Patients with silicosis are at high risk for developing TB. This
is probably caused by silica’s interference with the body’s
ability to ward off the bacteria that cause tuberculosis.
References:


